Doctors spend a decade in training to earn a high income…only to turn around and spend the next three decades handing a disproportionate share of it to the IRS. This is largely a consequence of being subject to a system that was built to help you, sure, but was never designed with you in mind.
The average physician earned $374,000 in 2024, up from $363,000 the year before — a modest 2.9% increase.
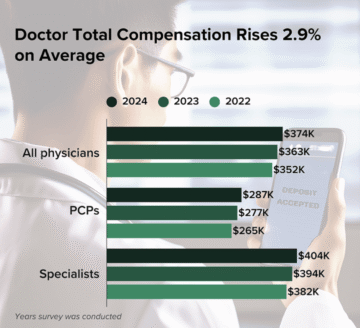
Source: Medscape
Physicians face effective tax rates of 30% to 40% when federal, state, and FICA taxes are combined, leaving roughly 60 to 70 cents on every dollar earned.
The average medical practice overpays the IRS between $15,000 and $50,000 every year through missed deductions and an absent strategy. 82% of physicians believe they’re overpaying in taxes, which is nearly double the rate of the general American public.
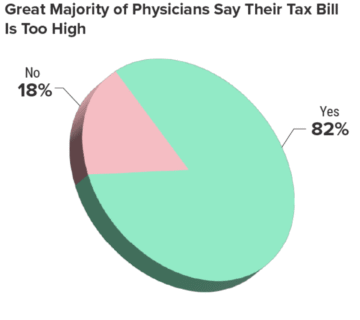 Source: Medscape
Source: Medscape
Over a 30-year career, that’s anywhere from $450,000 to $1.5 million that compounded for someone else. Specifically, the federal government.
Last month, Dr. Applegate (from Doc Wealth fame, a physician-founded tax planning firm) and I hosted a live webinar going through exactly where the money goes and how to stop the bleeding.
Here’s what we covered and more.
In case you missed it: You Didn’t Survive Residency to Overpay the IRS
Your March Appointment Needs A Revamp
The once-a-year CPA model was designed for people with a W-2 and a mortgage. It was never built for someone with a hybrid income, a practice entity, real estate, student loans, and a six-figure retirement capacity sitting untouched.
52% of physicians said they were dissatisfied with their compensation in 2025, the lowest satisfaction rate in a decade of Medscape surveys.
A fair portion of that dissatisfaction belongs at the feet of the tax bill. Nearly 40% of physicians are now taking on outside paid work to supplement their income.
Moonlighting is one solution. Keeping more of what you already earn is another, and it asks considerably less of your Saturday mornings.
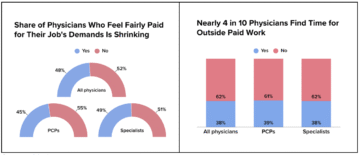
Source: Medscape
According to Doc Wealth’s physician survey, 93% of physicians reported poor communication and slow response times from their current CPA. 91% percent said their accountant does nothing beyond filing.
No entity structure review. No retirement plan design conversation. No flag on the $150,000 in tax-deferred capacity left on the table again this year.
This problem is as structural in nature as it is individualistic. Most generalist tax preparers run high volume across dozens of income profiles. They file what arrives. Physician-specific complexity demands a level of proactive, year-round engagement that a generalist practice is rarely set up to deliver.
Tax savings get created during the year. The best moves (say, adjusting retirement contributions, timing equipment purchases, structuring compensation, executing charitable gifts) all require action before December 31. After that date, the year is closed, and so are most of your options. April is a reporting deadline, not an extension to plan retroactively.
Here’s what you can do:
- Ask your CPA to walk you through what proactive strategies they initiated in the past 12 months. Filed returns tell you what happened. Planning conversations determine what happens next.
- Look for a physician-focused firm where CPAs, tax attorneys, and financial advisors work from a shared strategy. The coordination between those roles is where the savings live.
Our Guide to Tax Savings for Physicians
That Retirement Ceiling Is Actually the Floor
Most hospital-employed physicians know their 401(k) or 403(b). The 2026 contribution limit is $24,500, plus a $8,000 catch-up at 50 or older, or $11,250 for those aged 60–63, according to the IRA.
On a $500,000 income, that’s a 5% deferral rate that barely registers.
Any 1099 income (locum assignments, consulting fees, expert witness work, medical directorships, anything arriving on a 1099) opens eligibility for a Solo 401(k), operating entirely separately from your employer plan.
According to Medscape, the most common physician side gigs include medical consulting (25%), expert witness work (18%), and medical moonlighting (17%). Each and every one of those income streams generates 1099 income, and every one of them creates a separate retirement contribution bucket.
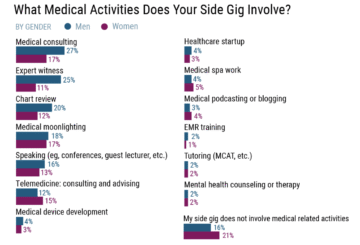
Source: Medscape
Self-employed physicians can also fund a SEP-IRA up to 25% of net self-employment earnings, capped at $72,000 for 2026. Stack those with an employer plan, and you’re already in a different ZIP code than your hospital plan alone.
Then there’s the cash balance plan, a defined benefit vehicle that has become something of a secret handshake in physician financial planning circles.
A physician earning $350,000 or more can often contribute $100,000 to $400,000 annually to a cash balance plan. Over 10 years, that builds roughly $3.4 million in tax-deferred assets, with annual deductible contributions that can exceed $300,000 when combined with a 401(k) and profit-sharing plan.
For married practice owners filing jointly, the SSTB phase-out ceiling is $544,600, which means a practice owner with $600,000 in net income who contributes $200,000 to a cash balance plan drops taxable income to $400,000, potentially restoring QBI deduction eligibility and adding another $80,000 in tax savings on top of the contribution deduction itself.
The Backdoor Roth IRA fills the gap for high earners blocked from direct Roth contributions. Contribute to a traditional IRA, convert it, and the Roth door stays open. The Mega Backdoor Roth goes a step further, routing after-tax 401(k) contributions through an in-plan Roth conversion.
The mechanics require attention, of course. Pre-existing pre-tax IRA balances can trigger the pro-rata rule and make conversions unexpectedly taxable.
That’s precisely the kind of landmine that surfaces when your tax advisor meets you once a year and doesn’t know the full picture.
Here’s what you can do:
- Calculate your actual deferrals versus your total eligible capacity across all available vehicles. The gap is usually enlightening.
- If you carry any 1099 income, open a Solo 401(k) before year-end. Contributions are deductible dollar-for-dollar from taxable income.
- Ask a physician-focused advisor for a cash balance plan feasibility study if your practice nets $300,000 or more annually.
Also read: Backdoor Roth vs Taxable Investing for High Earners
S-Corp It Up
Practice owners and independent contractors with meaningful 1099 income face a self-employment tax bill that multiplies quietly in the corner.
As a sole proprietor or single-member LLC, every dollar of net self-employment income takes a 15.3% hit up to the Social Security wage base, then 2.9% on everything above it.
An S-Corporation changes that calculation. Income gets split between W-2 wages (which carry payroll taxes) and owner distributions (which do not).
If your practice nets $600,000 and you set a reasonable W-2 salary of $300,000, the remaining $300,000 comes out as distributions, saving roughly $45,900 per year in self-employment taxes. For most practice owners, that’s $30,000 to $50,000 in annual savings simply from structuring income correctly.
The IRS requires the W-2 portion to represent reasonable compensation for your actual services, calibrated to your specialty.
What’s reasonable is well-documented by specialty and has to be supported. A physician-focused CPA can model the right number, and the savings almost always justify the administrative overhead of running the election.
Beyond the S-Corp, employing a spouse or adult children in the practice opens additional territory. A spouse on payroll can contribute up to $72,000 to their own retirement plan. Children can earn up to roughly $14,000 tax-free under the standard deduction, and those wages are deductible business expenses at the practice level.
Here’s what you can do:
- Have your CPA model the S-Corp election against your current structure using your actual income figures. Physicians filing as sole proprietors or single-member LLCs with $200,000 or more in net income will almost always find the election favorable.
- Document your reasonable compensation rationale by specialty. This is standard practice, and having it on file removes ambiguity.
Also read: 50 Boring Businesses to Invest in or Start: A Comprehensive List
Ben Franklin Never Had a Cost Segregation Study
He knew about death and taxes, sure. He never owned a medical office building.
Standard depreciation on a commercial building spreads the deduction across 39 years. On a $2 million purchase, that’s roughly $38,500 annually. Functional, but it’s slow money.
A cost segregation study runs an engineering analysis that reclassifies a portion of the building’s cost into shorter-life assets — electrical systems, plumbing, flooring, specialty fixtures. Those components depreciate over 5, 7, or 15 years (PDF) instead of 39.
Combined with 100% bonus depreciation, that reclassification can generate an $840,000 first-year deduction on a $2 million building, saving approximately $310,800 at the 37% rate.
The cost of the study itself runs $3,000 to $5,000. The ROI on that is difficult to replicate anywhere else in the tax code.
As for equipment, Section 179 allows deductions of up to $2,560,000 in qualifying purchases in 2026. The One Big Beautiful Bill Act permanently restored 100% bonus depreciation fo new equipment placed in service.
A $50,000 ultrasound machine purchased and placed in service before December 31 generates a $50,000 deduction this year instead of being depreciated across its useful life; that’s $18,500 in immediate savings at the 37% rate. The “placed in service” date is what triggers it. Miss it by a day, and the deduction waits 12 months.
Here’s what you can do:
- If you own or are acquiring commercial property used in your practice, order a cost segregation study before filing your return for that year. On any building above $500,000, the study pays for itself many times over.
- For major equipment purchases, nail down the placed-in-service date with your CPA in November — with enough runway to act before year-end.
The HSA Is Actually a Retirement Account
For most physicians, Health Savings Accounts get filed under “healthcare savings”. That’s underselling them considerably.
The architecture is genuinely magical. Contributions are tax-deductible going in, growth is tax-free inside the account, and qualified medical expense withdrawals are tax-free on the way out. No other account in the U.S. tax code runs all three. For 2026, the family contribution limit rises to $8,750, with a $1,000 catch-up for those 55 and older.
At a 7% annual return, an invested HSA grows to roughly $340,000 over 20 years and $860,000 over 30.
Strategists pay current medical costs out of pocket when cash flow allows, and leave the HSA untouched to compound. When you eventually want to access it, you can reimburse yourself tax-free for any qualified expense paid out of pocket, going back years, with receipts and no expiration on the clock.
After 65, unqualified withdrawals are taxed as ordinary income with no penalty. On the ground floor, this account essentially behaves like a traditional IRA.
The ceiling is considerably higher. You need enrollment in a qualifying high-deductible health plan to contribute. Medical graduates in 2024 carried an average loan balance of $216,659, with 32% of them owing more than $250,000.
For physicians managing that kind of debt load on an attending salary, every tax-efficient dollar of headroom matters.
Here’s what you should do:
- If you’re on a qualifying HDHP, max your HSA contribution every year without exception.
- Keep a running document of out-of-pocket medical expenses with dates and amounts. That’s your future tax-free withdrawal justification, collectible retroactively with no deadline pressure.
Learn more about what the HSA is
Stop Donating Cash — The IRS Is Watching
Physicians give generously. Cash donations are the default…which are the most expensive way to give.
Donating appreciated securities to a donor-advised fund instead of selling them first removes capital gains from the equation entirely.
Say you hold a position worth $150,000 with a $50,000 cost basis. Sell it first, and you owe capital gains tax on $100,000 of appreciation. Donate the shares directly to a DAF (donor-advised fund) instead, deduct the full $150,000 at fair market value, and pay zero capital gains.
At a 35% income tax rate, that’s $52,500 in income tax savings plus roughly $20,000 in avoided capital gains amounting to a $72,500 total benefit on a single gift.
A DAF also lets you front-load giving in a high-income year and distribute grants to specific charities over time. The deduction registers when money enters the fund, not when it exits.
The One Big Beautiful Bill Act added a provision for those taking the standard deduction: up to $1,000 (single) or $2,000 (married filing jointly) in charitable contributions can now be deducted without itemizing. It’s a modest number, but it’s free.
For physicians 70 and older, Qualified Charitable Distributions allow up to $111,000 annually to transfer directly from an IRA to a qualifying charity, satisfying required minimum distributions without the distribution ever appearing as taxable income.
Here’s what you can do:
- Open a donor-advised fund. Transfer appreciated securities rather than writing checks. The charity receives the same amount. Your tax bill takes a meaningful hit.
- If you’re 70½ or older, ask your advisor whether a QCD strategy makes sense alongside your RMD situation. It frequently does.
Learn more: Leveraging DAFs and QCDs for Tax-Effective Donations
One Big Beautiful Bill: What Changed, What Didn’t, and What’s Urgent
The One Big Beautiful Bill Act, signed in July 2025, is more than a 1,000 pages long. Here’s what deserves your attention:
- The TCJA tax brackets are permanent. The 37% top rate no longer reverts to 39.6% in 2026, which had been the scheduled outcome. For physicians above the top-bracket thresholds, that removes a significant planning variable and allows long-term projections to run with one fewer moving piece.
- The SALT deduction cap has been temporarily doubled to $20,000 for single filers and $40,000 for married couples, through 2030. It phases out at $250,000 for single filers and $500,000 for joint filers. For physicians earning in the $300,000 to $500,000 adjusted gross income range and living in high-tax states, the doubled SALT cap provides tangible relief.
- The lifetime estate and gift tax exemption moved to $15 million per person, indexed for inflation, permanently. If you have been postponing gifting strategies because the exemption was scheduled to drop in 2026, that pressure is gone.
- Dependent care FSA limits rose from $5,000 to $7,500 starting in 2026. Physicians, especially in dual-income households, carry significant childcare costs. That extra $2,500 in pre-tax FSA capacity is something.
- The student loan provision deserves its own flag. Beginning in 2026, most Income-Driven Repayment forgiveness becomes taxable. A $200,000 balance forgiven could generate a $70,000 or more federal tax bill. Public Service Loan Forgiveness remains tax-free. If you’re on an IDR plan with a substantial balance, the strategy you had in place before this law passed needs to be revisited.
Here’s what you should do:
- If you’re on an IDR plan, model out the taxability of your projected forgiveness with a physician-focused tax advisor before the end of this planning year.
- Increase your dependent care FSA contribution to the new $7,500 limit in 2026 if you have qualifying childcare expenses.
How does the One Big Beautiful Bill Act Affect High-Income Individuals and Taxpayers?
$40,000 Saved Per Year Doesn’t Stay $40,000
$40,000 saved annually in taxes, invested at 7% per year, grows to roughly $3.8 million over 30 years. That’s compound interest doing what compound interest does. Einstein may or may not have called it the eighth wonder of the world (allegedly) (alleged by whom? Me).
Physicians can overpay by $25,000 to $75,000 in a single year simply by missing key deductions or failing to optimize their strategies.
In 2024, nearly 70% of physicians reported either flat earnings or only single-digit income increases — a sign that post-pandemic salary gains have largely tapered off. About half of all medical specialties reported a compensation gain of 2% or less, and several specialties saw declines.
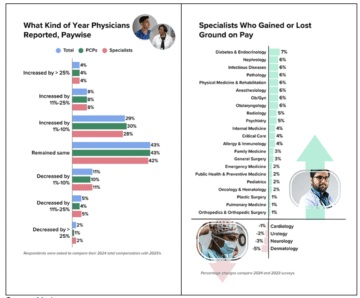
Source: Medscape
The hope of squeezing more out of clinical hours is increasingly grim. The hope of keeping more of what you already earn is entirely different.
The strategies in this article are mainstream, well-documented, and IRS-sanctioned. The physicians who use them have advisors who see the full picture and plan throughout the year. The complexity of physician compensation requires more than basic tax preparation.
It needs strategic tax management that coordinates with an overall financial plan.
Most physicians who overpay the IRS do so across multiple fronts simultaneously. Their entity structure could be wrong. Their retirement capacity is untapped. Their real estate deductions go unclaimed. Each one is a separate leak. Together they add up to a career’s worth of avoidable loss.
In case you missed it: Planting Your Money Trees
Frequently Asked Questions
How much do physicians overpay in taxes each year?
The average medical practice overpays the IRS between $15,000 and $50,000 annually through missed deductions and absent strategy. According to the Medscape Physicians and Taxes Report 2025, 82% of physicians believe they’re overpaying in taxes, nearly double the rate of the general American public. For physicians earning $500,000 or more, the gap between what they owe and what a well-planned return produces can exceed $100,000 per year.
What is the effective tax rate for physicians?
When federal income tax, state income tax, and FICA taxes are combined, physicians face effective tax rates of 40% to 50%, sometimes higher depending on state of practice and income composition. A physician in California or New York earning $600,000 will pay meaningfully more than one in Florida or Texas earning the same amount, purely due to state income tax. Proactive planning can bring that effective rate down significantly without changing income levels.
Why do physicians overpay the IRS?
Most physicians are employed, meaning unreimbursed work-related expenses are nondeductible and benefit options are limited to what an employer offers. Add in limited control over income timing, the pressure of student debt, and a general lack of bandwidth to engage with a complex tax code, and the conditions for overpayment are baked in from the start. Most generalist CPAs compound the problem by filing returns rather than planning proactively. According to Doc Wealth’s physician survey, 91% of physicians said their accountant does nothing beyond filing.
What retirement accounts can physicians use to reduce taxes?
Physicians have access to more tax-deferred vehicles than most professionals realize. Hospital-employed physicians can contribute $24,500 to a 401(k) or 403(b) in 2026, with an $8,000 catch-up at 50 or older. Any 1099 income opens a Solo 401(k), which allows up to $70,000 in total contributions for 2026. Self-employed physicians can fund a SEP-IRA up to $72,000. A cash balance plan stacked on top of a 401(k) can shelter $250,000 to $350,000 or more per year from current taxation for physicians over 40. Over a 20-year career, the tax-free growth on Mega Backdoor Roth contributions alone can be worth $500,000 to $2,000,000 in retirement.
Does the S-Corp election actually save physicians money?
For physicians with $100,000 or more in net self-employment income, the answer is almost always yes. Without an S-Corp, you pay 15.3% self-employment tax on all net profits. With one, you pay yourself a reasonable salary subject to payroll taxes and take remaining profits as distributions with no self-employment tax. On $300,000 in distributions, that’s roughly $45,900 saved annually, before any other strategy enters the picture. The key is setting a defensible W-2 salary calibrated to your specialty and documenting the rationale.
What is a cash balance plan and should physicians use one?
A cash balance plan is a defined benefit retirement plan that allows annual contributions well above the 401(k) limit. A physician over 50 can potentially shelter $300,000 or more per year from current taxation when a cash balance plan is stacked on top of a 401(k) and profit-sharing plan. Over a decade, that builds roughly $3.4 million in tax-deferred assets. For married practice owners filing jointly in 2026, the SSTB phase-out ceiling sits at $544,600, meaning a physician earning $600,000 who contributes $200,000 to a cash balance plan drops taxable income to $400,000, potentially unlocking a 20% QBI deduction worth an additional $80,000.
Can physicians deduct charitable donations without itemizing in 2026?
Yes, under the One Big Beautiful Bill Act. Physicians taking the standard deduction can now deduct up to $1,000 in charitable contributions if single, or $2,000 if married filing jointly, without itemizing. For those who do itemize, donating appreciated securities to a donor-advised fund instead of cash avoids capital gains tax entirely while generating a deduction at the full fair market value of the securities. On a $150,000 position with a $50,000 cost basis, that structure produces roughly $72,500 in combined tax savings on a single transaction.
What does the One Big Beautiful Bill Act change for physicians in 2026?
Several things worth knowing. The TCJA tax brackets are now permanent, so the 37% top rate stays put rather than reverting to 39.6%. The SALT deduction cap doubles temporarily to $40,000 for married filers through 2030, with a phase-out starting at $500,000 of joint income. The lifetime estate and gift tax exemption increased to $15 million per person, permanently. 100% bonus depreciation is restored for new equipment placed in service. And starting in 2026, most Income-Driven Repayment loan forgiveness becomes taxable. A $200,000 forgiven balance could generate a $70,000 or more federal tax bill. Physicians on IDR plans should treat that last point as urgent and revisit their loan strategy immediately.
Should physicians use an HSA as a retirement account?
Physicians enrolled in a qualifying high-deductible health plan should be funding their HSA to the maximum and leaving it invested. The 2026 family contribution limit is $8,750, with a $1,000 catch-up at 55 or older. At a 7% annual return, a fully funded family HSA grows to roughly $340,000 over 20 years and $860,000 over 30. Qualified medical expense withdrawals are tax-free at any age. After 65, unqualified withdrawals are taxed as ordinary income with no penalty, meaning the account’s floor is a traditional IRA and its ceiling is considerably higher.
What should physicians look for in a tax advisor?
The real issue for most physicians is the absence of a proactive strategy that identifies savings long before year-end. Even well-managed practices often leave tens of thousands of dollars on the table each year because their tax planning is reactive. A physician-focused advisor should be initiating quarterly conversations about entity structure, retirement plan design, charitable strategy, and equipment timing without prompting. Firms that combine CPAs, tax attorneys, and financial advisors under one roof and serve exclusively physician clients tend to produce the most coordinated outcomes. The cost of the right advisor is almost always smaller than the tax savings they generate












